 Research finds use of smaller, self-contained devices reduced complications for up to 18 months compared with conventional designs
Research finds use of smaller, self-contained devices reduced complications for up to 18 months compared with conventional designs
The findings of the research, led by Ohio-based Cleveland Clinic, appeared in the journal Heart Rhythm. The study compared patient outcomes for those fitted with new ‘leadless’ pacemakers compared with more conventional ‘transvenous’ designs.
Lead author Daniel Cantillon, research director for Cardiac Electrophysiology and Pacing at Cleveland Clinic, said: “The data from this study is encouraging, and we expect complications from leadless pacemakers to continue to decline as the technology improves and physicians gain experience implanting these devices.
“While this research shows benefit for leadless pacing, we must keep in mind that the field is still too young to compare the long-term results of this technology, the implications of which will not be fully understood for at least another decade.”
More than one million pacemakers are implanted annually worldwide, providing electrical stimulation to regulate a patient’s heartbeat. Conventional models are surgically placed under the skin of the chest and connected to the heart via a wire that stretches from the shoulder vein to the heart. These leads – and their surgical implantation – are the most common source of complications among pacemaker recipients as a whole, occurring in up to 12% of this group, according to previous research.
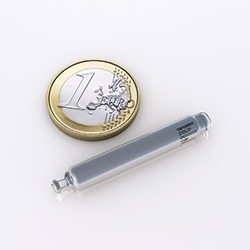
Leadless pacemakers, by contrast, do not need wires. These small, self-contained devices—about one-tenth of the size of a traditional pacemaker—are placed directly into the heart using a catheter that is carried from the leg to the heart via the thigh’s femoral vein. The first leadless pacemaker was introduced in 2014 and approved by the US Food & Drug Administration (FDA) two years later.
The new multicentre study compared short- and mid-term complications between 718 patients receiving the Nanostim leadless pacemaker and 1,436 patients with conventional (transvenous) pacemakers. Leadless pacemaker patient data was taken from the LEADLESS II trial, a prospective, nonrandomised, multicentre clinical trial. Transvenous patient data were obtained from Truven Health MarketScan claims databases for patients implanted with single-chamber pacemakers between April 2010 and March 2014 and more than one year of pre-implant enrolment data. Statistical methods were used to match patients between the two groups to compare the outcomes of a leadless versus traditional pacemaker with other key clinical variables being equal.
At one month, the study found that patients receiving one type of leadless pacemaker (Nanostim) overall had fewer complications (5.8 % vs. 9.4%). Leadless pacemakers eliminated lead and pocket complications, including infection. By comparison, complications among traditional pacemaker recipients included lead complications (3.62%), pocket complications (0.42%) and infection (1.74%).
There were no significant differences between the groups in regard to rates of vascular complications, electrode dislodgement, or generator complications. However, the study did find that those receiving leadless pacemakers had an increased risk of developing pericardial effusion – bleeding between the heart and the sac that surrounds it—of 1.53% vs. 0.35%. These complications were uncommon but serious, and sometimes required surgery.
Beyond one month and up to 18 months of follow-up, leadless patients continued to experience overall fewer complications than transvenous patients (0.56% vs. 4.94%). In the conventional pacemaker group, a number of complications were wholly absent from the leadless group, including lead-related complications, electrode dislodgement, infection, and pocket complications.









