
As a result of the COVID-19 pandemic, the increasing uptake of paediatric electrophysiology (EP) telehealth services has demonstrated clear ability to deliver healthcare for a pathologically and geographically diverse group of patients, who mostly report satisfaction with the service. This is the main concluding finding of a review published in the Cardiovascular Digital Health Journal in January.
The COVID-19 pandemic has heavily influenced healthcare access, with telehealth visits growing exponentially, according to the authors of the review, Jennifer Silva (Washington University School of Medicine, St Louis, USA) et al. In this review, Silva et al set out to investigate both the implementation and early experience of the paediatric EP telehealth programme, which was implemented in the US Midwest during the pandemic. Patient satisfaction, patient equity and inclusion (measured by geographical outreach), and sustainability were reported to be the primary areas of interest.
Patient data, including demographic testing and billing data from telehealth encounters between March and August 2020, were collected from a single paediatric EP group, and patients were asked to complete surveys regarding satisfaction. The data revealed a pathologically diverse patient population accessing telehealth services, with the most common health concerns named as inherited arrhythmia syndromes in 20% (n=23) of patients, and supraventricular/atrial tachycardias in 35% (n=41) of patients. A total of 118 patients were included in the analysis, consisting of 56% (n=66) females, with 64% (n=76) over the age of 10 and with 21% aged 6–9 years and 15% aged 0–5 years.
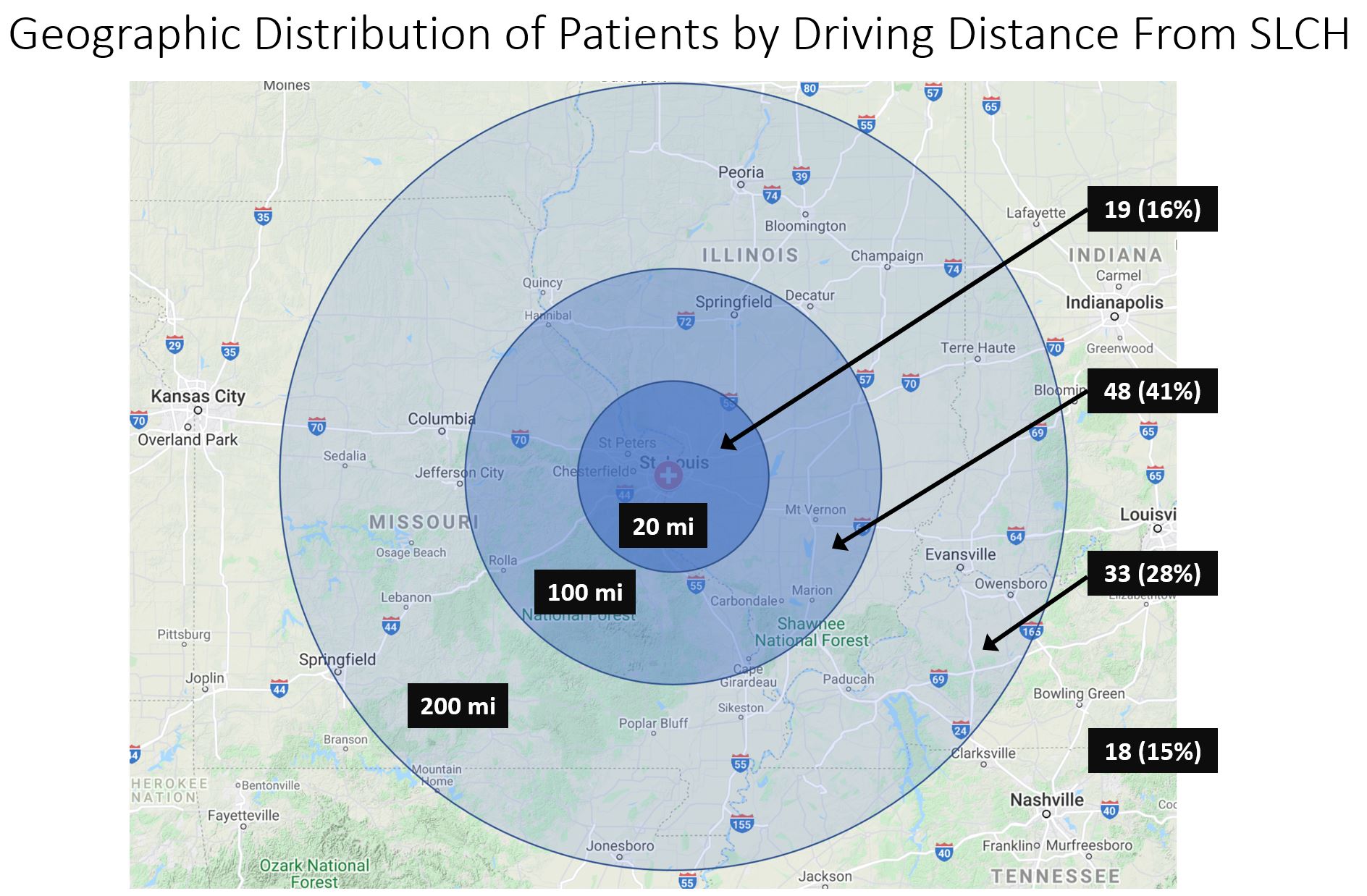
The authors report that 43% of patients live more than 100 miles away from the clinic, with the average distance being 95 miles (range 2.8–320 miles). Between the data collection dates, a total of 172 tests were performed, with 59% (n=102) at pre-visit and 31% (n=53) post-visit, also including 15 EP studies.
Speaking to Cardiac Rhythm News, Silva relayed “While there is a perception that telehealth visits may be difficult to implement in the very young and very old, we found that age was not a deterrent to the use of telehealth in our young population.”
For billing purposes, terminology codes were predominately used in 78% (n=92) of patient cases. Additionally, for visits, the work relative value unit (wRVU) was 220.50 wRVU, and 325.10 wRVU for testing. Patient satisfaction regarding the telehealth appointment was reported in 98% of patient cases, with 99% of patients demonstrating a clear understanding of their diagnosis.
Silva et al conclude that EP telehealth clinics can offer healthcare for a pathologically and geographically diverse group of patients who illustrated satisfaction regarding telehealth.
Lastly, the authors highlight that the review demonstrates significant downstream testing, and subsequent wRVU generation, suggesting financial sustainability of paediatric EP telehealth. Looking into the future, Silva states “Our following study, supported by the American College of Cardiology (Missouri Chapter) is designed to assess various digital health technologies and understand if they can further augment telehealth visits through the integration of real-time electrocardiography, pulse-oximetry, and cardiac/pulmonary auscultation.”











