This article was sponsored by Abbott.
Left ventricular assist devices (LVAD) are mechanical pumps that are implanted inside a person’s chest to help their weakened heart ventricle pump blood throughout the body. The mechanical device supports the left heart chamber that pumps blood through the body.
Unlike an artificial heart, a LVAD assists the heart instead of replacing it. This is a lifesaving therapy for patients awaiting a heart transplant and is termed “bridge-to-transplant”. Patients use the LVAD until a heart becomes available and, in some cases, the LVAD is able to restore the failing heart, eliminating the need for a transplant.
LVADs may also be used as destination therapy, which is an alternative to transplant. Destination therapy is used for long-term support in some terminally ill patients whose condition makes them ineligible for heart transplant.
LVADs have been shown to be effective in patients with end stage heart failure who are unable to receive a heart transplant. Patients receiving LVADs can suffer from cardiac rhythm disorders. Permanent treatment with continuous-flow LVAD has been shown to improve survival and quality of life compared to drug therapy alone.1
Since the first LVAD device was implanted in a 37-year-old woman in 1966, LVADs have been improving patient outcomes.2

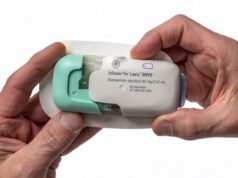
The Abbott HeartMate 3™ LVAD assists the heart in pumping blood around the body, increasing the oxygenation of organs. The device has Full MagLev™ Flow Technology, which provides better blood handling and reduces complications such as pump thrombosis, stroke and haemolysis. Two-year results from the Momentum 3 trial have shown superior survival free of disabling stroke or reoperation, with the overall rate of stroke being lower with HeartMate 3™ LVAD centrifugal-flow pump group when compared to the axial flow pump group.3 Reoperation for pump malfunction was also 90% less frequent for the HeartMate 3™ centrifugal-flow pump group than in the axial-flow pump group.
The HeartMate 3™ LVAD is the first implantable, continuous-flow heart pump that uses unique full magnetic levitation without the need for hydrodynamic contribution and has wide blood-flow passages to reduce shear stress, is essentially frictionless with no mechanical bearings and produces an intrinsic pulse to reduce stasis and avert thrombosis.4,5
Cardiac Rhythm News spoke to consultant cardiologist Steven Shaw (University of Manchester, UK) about what LVAD devices can offer.
LVADs offer support to patients with severe heart failure. How do they work?
To put it simply, LVADs take blood from the left ventricle that has not enough strength anymore and return it to the main artery of the body. This aims to restores an adequate cardiac output for the patient.

Which patients might receive or benefit from an LVAD device?
Patients with advanced heart failure due to severe left ventricular impairment are considered for LVADs. In the UK National Health Service (NHS), we are commissioned to implant them in patients who need a heart transplant but have not got time to wait. They can help to prolong life and restore a better quality of life in these patients. Indeed, it is now common for LVADs to be able to support patients for a time period measured in years.
Who is referring patients for LVAD implantation and when should a patient be referred?
Most patients get referred by their local consultant cardiologist or heart failure specialist nurse. Patients should be referred to an advanced heart failure centre if they remain symptomatic despite best efforts with conventional treatment, or there are signs of poor prognosis such as recurrent hospital admissions, high diuretic requirement, high B-type natriuretic peptide levels, kidney or liver impairment, high pulmonary pressure, etc. We prefer patients to be referred earlier rather than later.
Are there selection criteria to identify which patients are suitable?
Selection is a very complex process that is the responsibility of a transplant multidisciplinary heart failure team. Eligibility is based on whether the patient is regarded a transplant candidate. Suitability is defined by detailed tests which include imaging, a haemodynamic study of the heart (a right heart catheter) and blood tests.
What are the drawbacks of LVAD devices?
The cost is high, which means the selection criteria in the NHS is strict and we cannot therefore implant everyone we could otherwise. There are some important lifestyle limitations. You cannot perform contact sports, you cannot immerse yourself in water (i.e. go swimming) and you must always be connected to power.
The treatment is not without its risks and complications can happen. Some people have survived over a decade on LVAD support which is fantastic but, overall, they are yet to be able to match the long-term outcomes of transplantation.
What is the difference between ‘bridge to transplant’ and ‘destination therapy’?
Bridge to transplant means we are using the LVAD to keep a patient stable until a heart transplant can be done. Destination Therapy means that the LVAD is intended from the outset to be long-term therapy instead of transplant. The NHS does not fund this indication at present but it is funded in most of the other European health care systems.
How does the HeartMate 3TM device differ from other devices and what does the latest clinical evidence teach us?
The design of the pump in the HeartMate 3™ [device] is rather unique and has been designed to minimise complication rates. The rotor is fully levitated in a magnetic field, which means it is essentially frictionless. The latest evidence (which comes from one of the largest ever research study of LVADs) shows that the risk of stroke has been halved [10.1% vs. 19.2%] compared to its predecessor (the HeartMate IITM device) and that blood clots within the pump have been almost completely abolished.3
How should the different specialties work together for the best outcomes in LVAD patients?
In Manchester [UK] we have heavily promoted the importance of a multispecialty approach to managing VAD patients. In our outpatient VAD clinics, we encourage cardiologists, specialist VAD nurses, physiotherapists, dieticians, psychologists, and social workers to all collaborate together in a collective effort to aid the recovery and wellbeing of patients. We think this approach is one of the reasons that our outcomes are well recognised.
References
- Abraham WT, Smith SA. Devices in the management of advanced, chronic heart failure. Nature Reviews Cardiology. 2013;10(2):98-110.
- Kirklin, JK; Naftel, DC. “Mechanical circulatory support: registering a therapy in evolution”. Circulation: Heart Failure. 1 (3): 200–5.
- Mehra, MR et al.Two-Year Outcomes with a Magnetically Levitated Cardiac Pump in Heart Failure N Engl J Med 2018; 378:1386-1395
- Heatley G, et al. Clinical trial design and rationale of the Multicenter Study of MagLev Technology in Patients Undergoing Mechanical Circulatory Support Therapy With HeartMate 3 (MOMENTUM 3) investigational device exemption clinical study protocol. J Heart Lung Transplant 2016;35:528-536
- Schmitto JD, et al. First implantation in man of a new magnetically levitated left ventricular assist device (HeartMate III). J Heart Lung Transplant 2015;34:858-860
Abbott
The Corporate Village, Da Vincilaan 11 Box F1, 1935 Zaventem, Belgium
Tel: +32 2 774 68 11
SJM.com
St. Jude Medical is now Abbott.
Brief Summary: Prior to using these devices, please review the User’s Manual for a complete listing of indications, contraindications, warnings, precautions, potential adverse events and directions for use.
™ Indicates a trademark of the Abbott group of companies.
© 2018 Abbott. All Rights Reserved.
28191-EM-HM3-0518-0065 | Information contained herein for use outside the U.S. only. Check the regulatory status of the device in areas where CE marking is not the regulation in force.